Living with diabetes involves managing various health aspects, and nerve damage is one type of complication. Diabetic neuropathy is a type of nerve damage that can occur if you have diabetes, affecting different parts of the body. Here is more information about the condition, including its causes, symptoms, and available treatment options:
What Is Diabetic Neuropathy?
Diabetic neuropathy is nerve damage caused by high blood sugar levels associated with diabetes, and it can affect nerves throughout your body. The most common form is peripheral neuropathy, which typically affects the feet and legs first, sometimes followed by the hands. Other types include autonomic neuropathy, which affects the nerves controlling internal organs, such as the heart, bladder, and digestive system. Proximal neuropathy is a rarer form that impacts nerves in the thighs, hips, or buttocks, often on one side of the body.
What Causes It?
The primary cause of diabetic neuropathy is prolonged exposure to high blood sugar, which can injure nerve fibers throughout your body. High glucose levels interfere with the nerves’ ability to transmit signals, while also weakening the walls of the small blood vessels that supply nerves with oxygen and nutrients. A combination of factors often contributes to the development of this condition.
Genetic predisposition can also play a part, making some individuals more susceptible to nerve damage than others. Lifestyle factors, such as smoking and alcohol consumption, further damage blood vessels and nerves, increasing the risk. Managing your blood sugar levels is a key step in preventing or slowing the progression of neuropathy.
What Are the Symptoms?
Symptoms vary depending on the type and the nerves affected, ranging from mild to severe. For peripheral neuropathy, common symptoms include numbness, tingling, or a burning sensation in the feet and hands. Autonomic neuropathy can present a wider range of symptoms, such as dizziness, changes in digestion, and problems with bladder control. Proximal neuropathy may cause severe pain in the hips and thighs, along with weakness in the legs.
What Are the Treatment Options?
Managing diabetic neuropathy focuses on slowing the progression of the disease and relieving pain, so a multi-faceted approach is often used. The first step is to bring blood sugar levels within a target range through lifestyle changes. Medical treatments can also help manage symptoms.
Physical Therapy
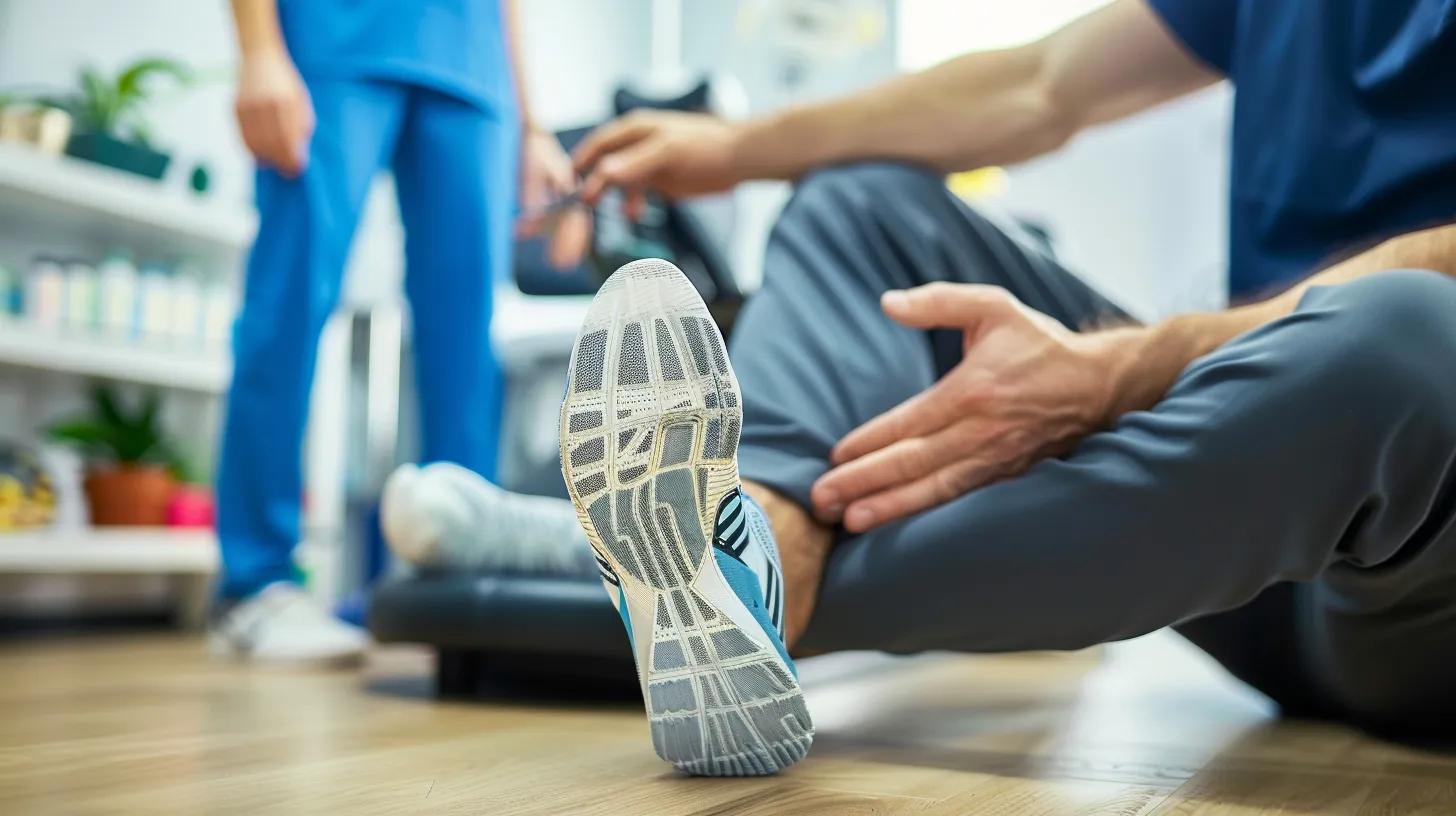
Physical therapy helps improve strength and balance, and it may also reduce some of the painful symptoms of neuropathy. A physical therapist can teach you exercises to maintain muscle function and mobility. This approach is beneficial for managing pain and improving your overall quality of life.
Medication
Certain medications are effective in relieving nerve pain, although they do not reverse the nerve damage itself. Antidepressants and anti-seizure medications are often prescribed because they can interfere with the pain signals sent by damaged nerves. Your doctor will determine the appropriate medication based on your symptoms and medical history.
Injections and Stimulation
For localized pain, nerve block injections with a local anesthetic provide temporary relief by interrupting the transmission of pain signals. Anti-inflammatory steroid injections may also be used to reduce inflammation around the nerves. In more severe cases, spinal cord stimulation, which uses an implanted device to send low levels of electricity to the spinal cord, may help mask pain signals.
Find Relief Today
If you are experiencing symptoms of diabetic neuropathy, it is beneficial to seek a medical evaluation. A healthcare professional can provide a diagnosis and recommend a treatment plan tailored to your specific needs. Taking action now can help you manage your symptoms and maintain your quality of life.