A functioning spine supports the body, facilitates movement, and protects the delicate nervous system. When structural components within the back sustain damage, the resulting discomfort frequently limits mobility and disrupts routine tasks. Many people face back issues at some point in their lives, and specific injuries like herniated discs require targeted interventions. Physical therapy provides a structured, non-surgical approach to managing these symptoms and restoring function.
What Is a Herniated Disc?
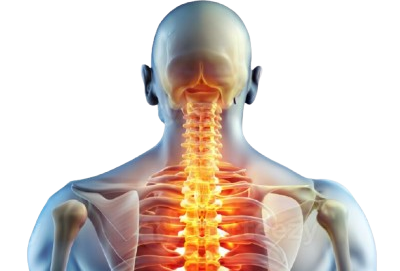
The human spine consists of a stacked column of bones called vertebrae, and between each of these individual bones rest circular, rubbery discs. These discs act as the body’s natural shock absorbers, cushioning the bones during walking, running, and jumping. Each disc features a distinct two-part structure. The center, called the nucleus, possesses a soft, jelly-like consistency. A tougher, rubbery exterior ring, known as the annulus, encases and protects this soft center.
A herniated disc occurs when a portion of the softer interior pushes through a crack or tear in the tough exterior ring. The displaced interior material protrudes into the spinal canal, and this canal offers very little extra space. Because of this limited space, the protruding material frequently presses directly against nearby spinal nerves. Nerve irritation leads to a specific set of symptoms. Depending on whether the injury occurs in the lower back or the neck, individuals routinely experience localized pain, tingling sensations, numbness, or weakness that radiates into the arms or legs.
How Is One Detected?
Several specific factors contribute to the breakdown of spinal discs. Gradual wear and tear stands as the leading cause of herniations. As people age, their spinal discs naturally lose water content. This dehydration makes the discs less flexible and more susceptible to tearing or rupturing with minor strains or twists. Physical exertion also triggers these structural failures. Using back muscles instead of leg muscles to lift heavy objects places excessive strain directly on the lower spine. Twisting or turning suddenly while bearing weight aggravates the structure further.
Medical professionals rely on comprehensive physical examinations and advanced imaging to confirm the presence of an injury. During a physical exam, the doctor tests a patient by having them perform simple movements. To verify the exact location of the damage, providers order MRI or X-ray scans. These sophisticated imaging tools reveal detailed pictures of the spine and highlight precisely where the protruding material makes contact with the nerves.
How Does Physical Therapy Treat It?
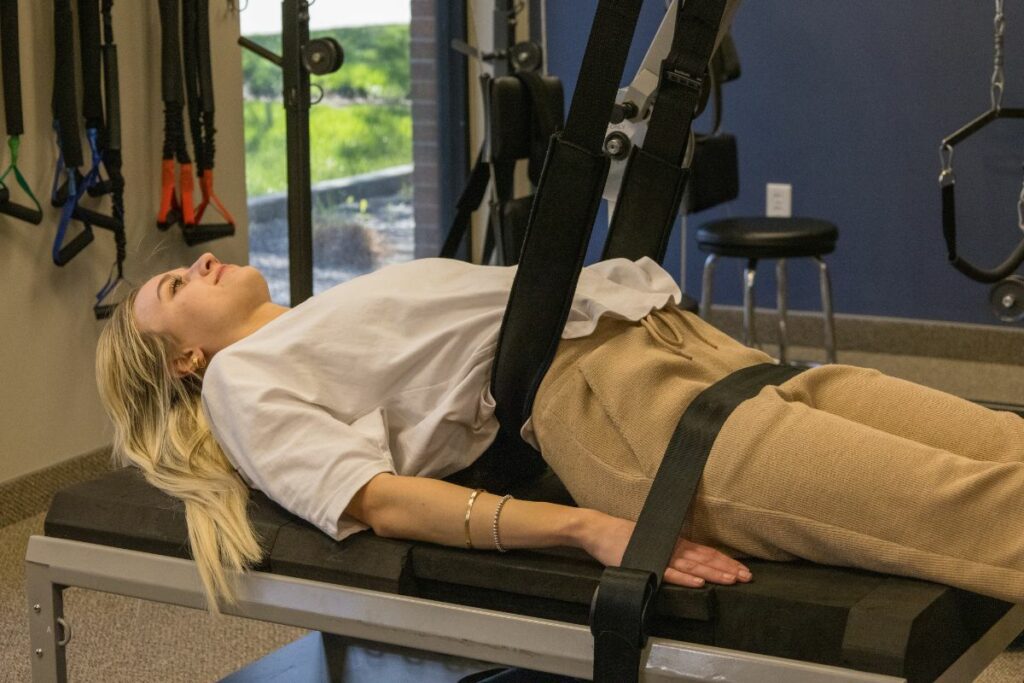
Initial management often involves modifying daily activities and avoiding movements that aggravate the pain. Physical therapy serves as a primary non-surgical pathway to recovery. Licensed therapists design customized exercise programs, tailored to the specific functional needs of each patient.
Active physical therapy emphasizes strengthening the core muscles, aiming to stabilize the spine. Stronger abdominal and back muscles can reduce the daily load placed on the spinal discs, and therapists may guide patients through specific stretching routines designed to improve flexibility in the lower back. Proper body mechanics training forms a major part of this education. Therapists can teach patients how to lift objects safely and other safe ways to maintain spinal health.
Seek Professional Therapeutic Treatment
Recovering from a spinal injury may require guided, professional care to avoid exacerbating the structural damage. A medical professional monitors progress accurately and adjusts the exercise regimen to match the patient’s healing timeline. Integrating ergonomic practices into daily life supports long-term recovery. By combining prescribed therapeutic exercises with mindful lifestyle adjustments, individuals can protect their backs from recurrent injuries and maintain sustained structural health.