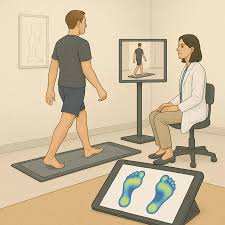
Podiatry focuses on diagnosing and treating disorders affecting the human foot and ankle, and this may involve gait or balance issues. Even if balance issues originate elsewhere, the feet frequently play a primary, fundamental role. Podiatrists examine these complex connections, and they develop plans to restore stability effectively. Here is more information about how podiatry addresses gait and balance issues:
Identifying Underlying Conditions
Systemic diseases affect the feet, and nerves can suffer significant damage early on. Diabetes may alter sensation in the lower extremities, leading to numbness or pain. Because sensation decreases, patients might not notice minor injuries or shifts in balance. This lack of feeling creates instability while walking on uneven surfaces.
When arthritis targets the joints, stiffness effectively limits the range of motion. Inflammation causes pain, and this discomfort forces changes in natural movement patterns. Through a comprehensive physical examination, a podiatrist identifies these specific mechanical restrictions. Addressing the source of pain improves overall stability significantly for the patient.
Analyzing Gait
Gait analysis involves a detailed observation of walking patterns to find irregularities. The doctor may watch the patient walk, and they note any mechanical deviations. Since alignment matters, technology tracks how the foot strikes the ground during movement. This data pinpoints the exact source of instability within the skeletal structure.
Providing Orthotics
Because feet differ, custom devices may support individual arch structures better than generic options. Mass-produced inserts might fail to correct specific irregularities found in many patients. A scan captures the foot’s shape, and a lab fabricates the device. These custom tools provide the exact support needed for the individual’s unique anatomy.
The device fits into the shoe, but it controls joint movement. While they feel rigid, orthotics distribute pressure evenly across the entire foot. Proper alignment is designed to reduce fatigue during daily activities and correct posture issues. Patients wear these inserts to maintain correct foot positioning throughout the day.
Rigid orthotics primarily control motion in the foot joints. Soft devices absorb shock, and they protect sensitive diabetic feet from pressure ulcers. If balance issues persist, the podiatrist adjusts the prescription for better stability. Choosing the right material depends on the patient’s weight and activity level.
Offering Physical Therapy
Since muscles support the skeletal structure, weakness often leads to poor balance. Targeted exercises strengthen the ankle and lower leg muscles to improve support. The patient repeats these movements, and stability improves over time with practice. A structured plan addresses specific muscular deficits that contribute to falls. Therapy plans in podiatry might include:
- Stretching tight calf muscles
- Strengthening toe flexor muscles
- Practicing single-leg stands
Regularly performing these exercises not only enhances balance but also reduces the risk of future injuries. Strength and flexibility are equally important, so combining both elements in a therapy plan promotes better overall outcomes. While progress may take time, consistent effort and adherence to the plan can lead to significant improvements in mobility and stability.
Find Podiatry Services Near You
Balance issues disrupt daily life, so professional evaluation remains a prudent step. Because falls pose risks, early intervention protects long-term mobility and independence. Schedule an appointment with a local podiatrist today to discuss your options. Taking action now may prevent future complications related to gait and stability.