Diabetic wound care involves specialized methods for treating wounds for individuals with diabetes. High blood sugar levels often lead to nerve damage and poor circulation, which can complicate the body’s natural healing processes. A minor cut or blister, which may be insignificant for others, can develop into a serious infection or a non-healing ulcer for a diabetic person. Proper management is fundamental to facilitating healing and preventing severe complications. Here’s information on effective strategies for diabetic wound care:
At-home Management Strategies
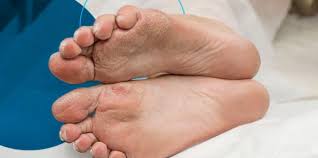
Diabetic ulcers are open sores or wounds that are common in individuals with diabetes, and they most often develop on the feet. Consistent and careful management at home is a key strategy for preventing the progression of diabetic wounds. This involves regular monitoring and adherence to specific care routines recommended by healthcare providers.
Why Ulcers Form
These ulcers result from a combination of factors, including nerve damage (neuropathy), which reduces sensation, and poor circulation, which impairs healing. Because a person may not feel a minor injury, like a blister or cut, it can go unnoticed and untreated. When wounds don’t heal, they lead to the formation of an ulcer.
What At-home Strategies Can Help
Daily self-checks are a key part of at-home diabetic wound care. Diabetic individuals should inspect their feet daily for any signs of injury, and they should keep their feet clean and dry to prevent bacterial growth. Some injuries to look for include:
- Cuts
- Blisters
- Redness
- Swelling
Managing blood sugar levels effectively helps diabetics keep their glucose levels stable, supporting their ability to heal. Wearing appropriate, well-fitting footwear that does not create pressure points is also a key preventative measure for some individuals.
Nonsurgical Strategies
When a diabetic wound develops, a healthcare professional may recommend nonsurgical treatments to promote healing and prevent infection. One primary approach is topical wound care, which involves cleaning the wound and applying specialized dressings. These dressings help maintain a moist environment conducive to healing while protecting the area from bacteria.
Another treatment is compression therapy, which uses special socks or bandages to improve blood flow in the lower legs. Improved circulation delivers more oxygen and nutrients to the wound site, which can accelerate the healing process. Oral or topical antibiotics may be prescribed if signs of infection are present or as a preventative measure.
Surgical Strategies
In cases where a diabetic wound is severe, surgical intervention may be necessary. Wounds that do not respond to nonsurgical treatments, especially when showing signs of deep infection, may benefit from surgical procedures like a debridement. Debridement is a standard procedure in which a surgeon removes dead, damaged, or infected tissue from a wound. This process cleans the wound bed and encourages the growth of healthy new tissue.
Some other surgical strategies for extensive ulcers may include:
- Skin Grafts: For deep ulcers, skin grafts or other advanced tissue products can cover the wound and stimulate closure.
- Amputation: For severe circumstances, when an infection has spread to the bone or threatens to become systemic, amputation may be required to prevent further complications.
Learn More About Diabetic Wound Care
Wound care is a complex but manageable aspect of living with diabetes. Staying informed about wound prevention and treatment strategies is a key part of ongoing diabetic health management. If you have concerns about a non-healing wound, contact a podiatrist for a consultation today. They can offer guidance on daily management and discuss what treatments are best for your needs.